Header logo
header top contact widget
Systemic Inflammation
Gum Disease & Prostrate Health
Posted on Apr 11, 2016 by William J. Claiborne, DDS MS
All bodies contain bacteria, some are even good for us. However, the human body was built to tackle the bad kind by sending white blood cells to battle the bacteria that can lead to infection. Although this is our body’s reaction to bacterial accumulation, some infection spreads beyond what white blood cells can handle.
This can be seen in a cut that goes unwashed and untreated. As bacteria multiply, inflammation sets in. This is what causes redness and swelling as white blood cells arrive to tackle the enemy. When the white blood cells are overwhelmed, an antibiotic may be needed to overcome the overload that the white blood cells cannot combat.
Systemic inflammation is similar, except it cannot be seen like the redness or swelling from a cut. This internal inflammation in the body can simmer without being obvious. With chronic inflammation, the reaction can’t turn itself off. While the white blood cells will back off when a cut heals, chronic inflammation inside the body continues for no reason.
Although invisible, this continual inflammation can contribute to a number of serious health problems. For example, research has found links between systemic inflammation and heart attacks, arthritis, diabetes, some cancers, preterm babies and even Alzheimer’s Disease. Now, researchers have begun to take a closer look at periodontal disease, a bacterial infection in the mouth, as being a potential trigger of internal inflammation.
As oral bacteria accumulate in the mouth, periodontal (gum) disease develops, thrives and spreads by eating away at gum tissues, tooth enamel and supporting bones. When the bacteria of gum disease enter the bloodstream through weakened gums, inflammatory reactions can create destruction far beyond the mouth.
Research now shows a potential link between oral bacteria and Prostatitis, an infection of the prostate. Prostatitis, an inflammatory disease, causes a frequent urge to urinate and a burning sensation or pain during urination.
The connection between periodontal disease bacteria and Prostatitis was recently noted in a study conducted at Case Western University. Researchers from Case Western’s School of Dental Medicine and the Case Medical Center’s Department of Urology & Pathology found that the symptoms of Prostatitis could be greatly improved by treating gum disease.
In their study, all participants had moderate to severe levels of periodontal disease. Those in the study also had inflammation of the prostrate gland with higher than normal prostate specific antigen (PSA) levels.
During the study, one group of participants were treated for gum disease while having prostrate symptoms and PSA levels monitored. The other group received no treatment for their gum disease while prostrate symptoms and PSA levels were monitored. Neither group was given treatment for their prostate conditions during the study.
PSA levels were measured in both groups after one month and again after two months. Researchers noted an overwhelming majority with noticeably lower PSA levels in the group who received treatment for gum disease. Hopefully, these findings can help Prostatitis patients achieve better treatment results.
As studies continue, it is obvious that your oral health is closely connected to your overall health. By avoiding bacteria overload in the mouth, you reduce the risk of triggering inflammatory reactions elsewhere in the body. Additionally, your smile will avoid problems that are time-consuming and expensive to treat.
Common symptoms of gum disease are tender gums that bleed when brushing, persistent bad breath, gums that turn red, gums that loosen from teeth and pus pockets that form at the base of teeth. If you have any of these symptoms, you should also know that periodontal disease is the leading cause of adult tooth loss in the U.S.
Obviously, the potent bacteria of gum disease is nothing to ignore, as research continues to find links between it and serious health problems. Take good care of your body AND your smile! Call 828-274-9440 to schedule a thorough examination. If signs of gum disease exist, we can make recommendations for treatment to restore your smile to a healthy state.
Can You Reverse Gum Disease?
Posted on Mar 03, 2016 by William J. Claiborne, DDS MS
Our bodies are miraculous machines. They not only provide mobility and enable various functions, the human body is designed to heal itself.
When bacteria enter the body, white blood cells are the microscopic soldiers that surge in for battle. Their job is to attack the bacteria and destroy it. As with any battle, however, when the odds are in favor of the enemy, the ‘good guys’ don’t always win.
Bacteria reproduce very rapidly. When they become too much for your body’s defense mechanism to overcome, infection begins. Just as a cut or scrape on the skin can become infected, oral bacteria can cause infection in the mouth. This overload of bacteria can evolve into periodontal disease, which is an inflammation that attacks teeth, oral tissues and the bone structures that support teeth.
Gum disease is characterized by sore gums that bleed when brushing, persistent bad breath, gums that recede from teeth and turn red in color, and pus pockets that form on the gums at the base of some teeth. In latter stages, gum disease will cause teeth to loosen and eventually require removal.
Most gum disease occurs because people are often unaware that bleeding gums or gum recession is not normal. Insufficient brushing, failing to floss and missing 6-month dental cleanings can lead to a build-up of bacteria that forms, at first, plaque. This is a sticky film you feel on teeth. When plaque is not removed on a regular basis, it forms a cement-hard colony of oral bacteria, known as tartar or calculus.
As your mouth is enduring the repercussions of oral bacteria accumulation, gum tissues and tooth enamel are being eaten away by the bacteria. There is a point where only dental treatment can eliminate the bacterial onslaught, especially when it has penetrated below the gum line. However, with prompt attention and proper measures, you can halt and reverse the need for dental treatment and the progression of gum disease.
Gingivitis is the initial stage of gum disease. Your symptoms will probably include gums that are tender in spots and some bleeding when you brush. These are warning signs that signal an immediate need for attention.
Begin by twice daily brushing with a soft bristle tooth brush and use a fluoridated tooth paste. Brush for at least two minutes per time. Floss daily. Be sure not to pop the floss between teeth to avoid damaging the gums. Move the floss in a back-&-forth motion between teeth to ease it down so you can scrape the sides of each tooth.
You can remove a tremendous amount of oral bacteria by using a tongue scrapper daily. Or, brush your tongue with your tooth brush at the end of each brushing. This helps to dislodge bacteria that is embedded in the grooves of the tongue.
Drink lots of water during the day. This will aid saliva flow that is designed to move oral bacteria from your mouth on a consistent basis. Avoid foods and beverages that are drying to oral tissues. These include coffee, colas, alcohol and spicy foods. Also, try to minimize the amount of sugar and carbohydrates you consume. These foods energize the reproduction of oral bacteria.
If you smoke, consider using an oral rinse that will replenish the mouth with moisture. The chemicals in cigarette smoke are terribly drying to oral tissues. Some oral rinses are specifically designed for producing moisture. This is helpful since dryness provides oral bacteria with a favorable environment for reproduction.
When these steps are taken for initial levels of gingivitis, your gums should be less tender and bleeding should cease in a week or so. If you do not see improvement after 1-2 weeks of implementing these measures, see a Periodontal specialist as soon as possible. This dental specialist can determine the precise level of gum disease you are experiencing and provide appropriate treatment.
The key is to act sooner than later. Gum disease only worsens without treatment. In the U.S., it is the leading cause for adult tooth loss. Your natural teeth are precious and worth saving. With a healthy mouth, having your natural teeth all your life is a reasonable expectation.
The oral bacteria of gum disease is also harmful to your health in other ways, too. This bacteria has been known to trigger inflammatory reactions elsewhere in the body. It can contribute to heart disease, arthritis, diabetes, stroke, preterm babies and impotency.
Call 828-274-9440 if you have questions about your gums or if you are experiencing any symptoms associated with gum disease.
Research Closely Ties RA To Gum Disease
Posted on Feb 10, 2016 by William J. Claiborne, DDS MS
As a Periodontist, I treat all stages of periodontal (gum) disease. In early stages, the condition causes gums to bleed when brushing, bad breath and gum tenderness. As gum disease progresses, gums become red in color and pus pockets form at the base of teeth. Eventually, teeth loosen and may require removal. Gum disease, to no surprise, is the nation’s leading cause of adult tooth loss.
Over the years, research has found a correlation between the bacteria of periodontal disease and a number of serious health problems. Due to the inflammatory triggers associated with the oral bacteria of gum disease, it has been linked to heart disease, stroke, memory loss, preterm babies, diabetes and impotency.
For people who have rheumatoid arthritis (RA), the condition’s association with gum disease seems unlikely. Yet, research is showing a remarkably close connection.
It’s not only been determined that both gum disease and RA share a genetic likeness, their clinical makeup shows similar structures, primarily in pathogens. A pathogen is an agent in the body that causes disease or illness. The pathological processes that occurs in both gum disease and RA are almost identical.
While it is apparent that both conditions cause chronic inflammation in tissues that connect to bone, researchers have found that both diseases also have a similar inflammatory trigger. Also alike is the particular species of bacteria found in periodontally-diseased oral tissues and tissues that surround joints in those who suffer with RA.
RA is a debilitating disease that destroys joints. It is disabling and painful. In most cases, RA emerges gradually, often beginning with morning stiffness along with weak and aching muscles. Joint pain follows, with joints feeling sore and stiff. RA is typically found in the fingers, wrists, elbows, hips, knees, ankles, toes, shoulder and neck.
As inflammation from RA increases, joints become swollen with symptoms including fever, disfiguring of hands and feet, numbness and tingling. There is no cure for RA and lifelong treatment is required. Treatment may consist of medications, physical therapy, or even surgery.
Like RA, periodontal disease causes pain, swelling, and tenderness. As it worsens, the associatedinflammation can lead to destruction of the bone that supports teeth along with surrounding tissues.
In one study, a particular pathogen associated with periodontal disease was found to activate the same destructive process of rheumatoid arthritis. It has also been shown that, by treating periodontal disease in RA patients, RA symptoms often improve. This is likely due to the system’s reduced burden of oral inflammation.
What’s exciting about the findings of these research findings is how oral health correlates so closely to one’s overall health. Yet, it’s a bit scary at the same time. When you realize that the presence of gum disease can so greatly increase your risk for serious health conditions, it should send up alarms. However, even in this advanced age of modern medicine, nearly 75% of the U.S. adult population have some level of periodontal disease.
Help spread the word about the link between your oral health and a healthy body, especially to those you love. Emphasize the need for a thorough oral hygiene regimen at home as well as a commitment to 6-month dental check-ups and exams. If you have signs of gum disease (as mentioned above), seek treatment at your earliest convenience. Gum disease will only worsen and will require more treatment time and expense as it progresses.
Call 828-274-9440 to learn more.
How Gum Disease Forms – Dental Terms Made Easy
Posted on Jan 15, 2016 by William J. Claiborne, DDS MS
A friend who recently acquired a sail boat loves to talk about his new passion. Unfortunately, as he casually throws out terms such as halyard, fife rail, and jibe when describing his outings, I become “lost at sea” (pun intended!). Rather than stop his conversation at each unfamiliar term for an explanation, I tend to try to absorb what I can. More than not, I fail to truly grasp the actual picture of what he is sharing.
As a Periodontal Specialist, I have to continually remind myself that some dental terminology that’s second nature to me isn’t as clear to the patients with whom I’m communicating. Just as jibe means very little to me, terms like osseointegration and mandibular are not familiar ones, often leaving the patient drifting as the conversation begins to fall apart.
Although dental implant placement and gum recontouring are regular treatments our office provides, gum disease is the most frequent problem we treat. Gum disease in the U.S. affects over 70% of adults at some level. It is the leading cause of tooth loss and has been linked to heart disease, high blood pressure, stroke, memory loss, arthritis, diabetes, preterm babies and impotency.
Because gum disease (also known as periodontal disease), begins without obvious symptoms, people often ignore the warning signs, which merely allows the disease to progress further. In order to help people have a clear, concise picture of how gum disease forms, I’ve broken the stages down in language that removes dental jargon.
• Oral bacteria – We all have bacteria in our mouths. That’s normal. However, it’s the excess of bacteria that is at the root of the problem. When oral bacteria are not brushed, flossed or rinsed from the mouth properly and on a daily basis, they band together and form plaque.
• Plaque – This is a sticky film that coats teeth. It also covers the gums and tongue but is not as obvious as what can be felt by running the tongue over teeth. The presence of plaque means the mouth contains more bacteria than saliva flow can handle. When plaque is not removed, oral bacteria continue to reproduce, thrive and form calculus.
• Calculus – Also known as tartar, this is actually a hardened form of bacteria that emerges from plaque. As a condensed colony of bacteria, calculus attaches to teeth and can only be removed with special instruments used by dental professionals. This is why your 6-month check-ups and cleanings are so important. By scraping away buildup on a regular basis, you can halt damage to gums and enamel.
• Gingivitis – This is actually the first stage of gum disease. In this stage, oral bacteria are attacking gum tissues and tooth enamel as they reproduce at a rapid rate. Signs of gingivitis are gums that bleed when brushing, sore spots and frequent bad breath. It is this stage, however, that can be self-treated. That is to say that an immediate response with proper measures can combat the problem before it worsens. This includes a minimum of twice daily brushing (at least two minutes each time) with a soft to medium bristle tooth brush and flouridated tooth paste. Daily flossing is also needed to remove food particles and bacteria between teeth. Tongue scraping is advised, also. This removes oral bacteria that is embedded in the grooves of the tongue. When a tongue scraper is not available, brush the tongue with your tooth brush after brushing teeth. Be sure to get to the back of the tongue where the greatest concentration of bacteria live. Drink lots of water and swish daily with an oral rinse that kills bacteria and provides added protection to enamel.
• Periodontal (Gum) Disease – When gingivitis is not resolved, the next stage you can expect will be periodontal disease. This is when the bacteria have moved down into the gum tissues and are eating away at gums and tooth enamel at a rigorous rate. Typical symptoms are red and swollen gums, gums that bleed easily when brushing, 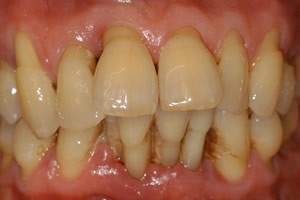 gums that pull away or loosen from teeth, exposing sensitive tooth root areas. Persistent bad breath is another symptom, which occurs even after brushing or chewing gum.
gums that pull away or loosen from teeth, exposing sensitive tooth root areas. Persistent bad breath is another symptom, which occurs even after brushing or chewing gum.
• Periodontitis – At this stage, gum disease is running rampant in your mouth. Gums are red and tender all the time. Pus pockets form at the base of some teeth. Some teeth will begin to loosen as bacteria eat away at the structures that support tooth roots. Eventually, some (or all) of your natural teeth will need to be removed.
I believe if the general population were more aware of the sequence that leads to full-blown gum disease, we’d have far less adults walking around with bacteria that causes internal inflammation. When oral bacteria enter the bloodstream through tears in diseased gum tissue, it can trigger inflammatory reactions that are the foundation of the severe health problems mentioned prior (heart disease, arthritis, etc.). We’d also have fewer adults dealing with the ordeals surrounding tooth loss.
I hope I’ve provided a helpful explanation of how oral bacteria progresses and how it effects your oral and overall health. For an examination to determine the health of your gums, along with recommended treatment options, call 828-274-9440 to request an appointment.
Remember, if you are having any symptoms, these will only worsen when treatment is delayed. This typically means more treatment time and greater expense.
Recent Posts
Categories
Archives
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- December 2016
- November 2016
- October 2016
- September 2016
- August 2016
- July 2016
- June 2016
- May 2016
- April 2016
- March 2016
- February 2016
- January 2016
- December 2015
- November 2015
- October 2015
- September 2015
- August 2015
- July 2015
- June 2015
- May 2015
- April 2015
- March 2015
- February 2015
- January 2015
- December 2014
- November 2014
- October 2014
- September 2014
- August 2014
- July 2014
- June 2014
- May 2014
- April 2014
- March 2014
- February 2014
- January 2014
- December 2013
- November 2013
- October 2013
- September 2013
- August 2013
- July 2013
- June 2013
- May 2013
- April 2013
- March 2013
- February 2013
- January 2013
- December 2012
- November 2012
- October 2012
- September 2012
- August 2012
- July 2012
- June 2012


